
The Duke Health Plans including Duke Basic, Duke Select, and Duke BCBS plans utilize the Express Scripts National Preferred Formulary to determine medication coverage. This formulary does not apply to those who are ≥65 years of age and covered by the Duke retiree plan.
Beginning January 1, 2017, 5 additional medications will be excluded. Additionally, two will be added back to coverage.
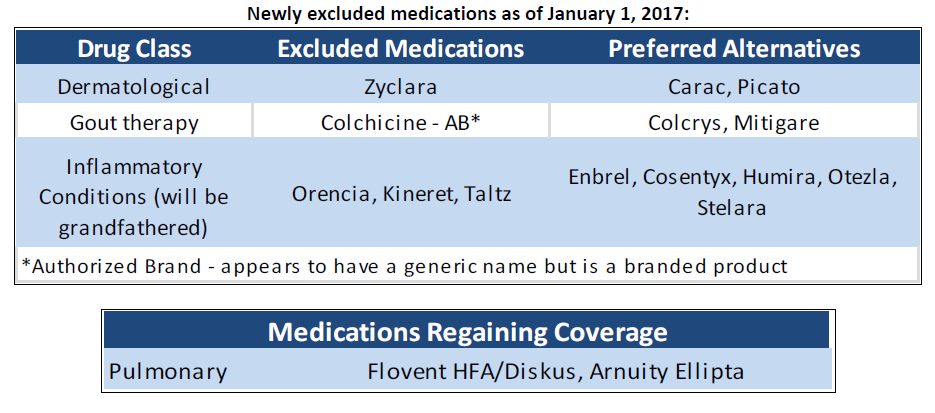
Of note, colchicine is a branded product which appears to have a generic name. There are NO generic forms of colchicine at this time. This is a strategy by pharma to circumvent plan design. This product is actually higher net cost than Mitigare or Colcrys for the Duke plan. Consider prescribing these medications over colchicine. Members currently taking Orencia, Kineret, or Taltz will be grandfathered and coverage will continue without disruption. The exclusion will only apply to those members new to these therapies. As in previous years, medications to treat weight loss and erectile dysfunction will not be covered. For any patient who is unable to use one of the alternative medications due to a clinical reason, a clinical exception process is in place. A provider or their staff may call 1-800-753-2851, provide the clinical rationale, and request coverage.
